Tooth pain has a way of stopping you in your tracks. Whether it’s a sharp sting when you sip your morning coffee or a dull ache that keeps you up at night, unusual dental symptoms can feel unsettling, especially when you’re not sure what’s causing them. If you’ve been wondering how do you know if you need a root canal, you’re not alone. It’s one of the most common questions dentists hear.
The truth is, only a dentist can confirm whether root canal therapy is the right treatment for you. But there are several warning signs that strongly suggest the inner pulp of a tooth may be inflamed or infected. In this post, we’ll walk through 6 of those signs, explain what they might mean, and help you understand when it’s time to pick up the phone and schedule an exam.
What Is a Root Canal and Why Would You Need One?
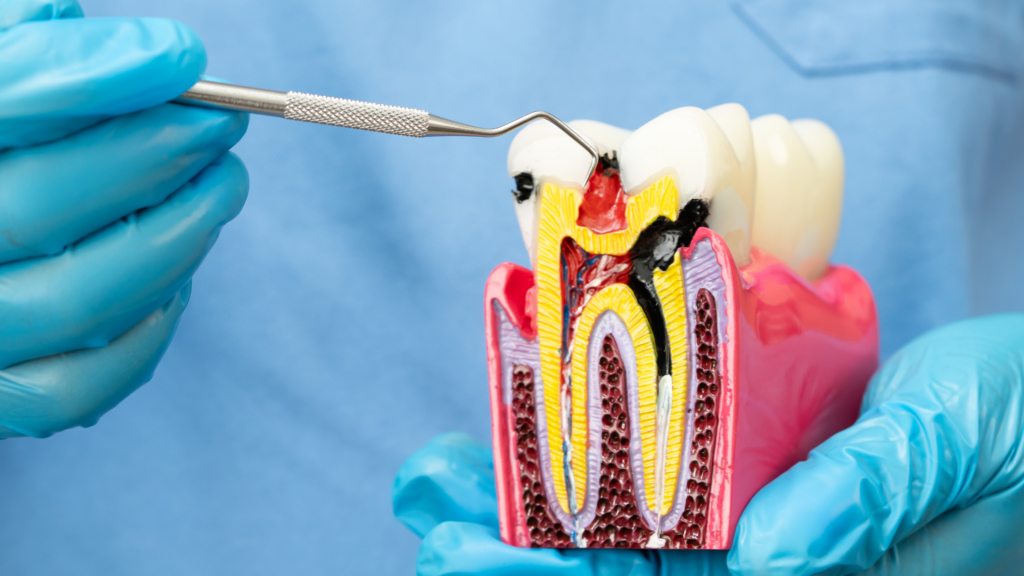
A root canal is a dental procedure designed to save a tooth that has become infected or severely damaged on the inside. Each tooth contains soft tissue called pulp, which runs through the root canals of the tooth. This pulp contains nerves and blood vessels that help the tooth develop. When it becomes infected or inflamed, it can cause significant pain and, if left untreated, serious complications.
Root canal treatment removes the damaged pulp, cleans and seals the inner chamber, and restores the tooth with a crown or filling so it can continue to function normally.
Common reasons a tooth may need root canal treatment include:
- Deep decay that has reached the pulp
- A cracked or chipped tooth that allows bacteria inside
- Repeated dental procedures on the same tooth over time
- Trauma to the tooth, even without visible cracking
Once the pulp is compromised, the body cannot heal it on its own. Recognizing the symptoms early makes a real difference in how straightforward treatment becomes.
1. Persistent Tooth Pain That Does Not Go Away
Ongoing pain is one of the most recognizable signs that something is wrong below the surface. It’s not the kind of fleeting twinge you might feel after eating something cold. This pain tends to stick around.
It may be constant or come and go throughout the day. Some people describe it as sharp and stabbing, while others feel a deep, throbbing ache or a dull pressure. The pain might seem to originate from a specific tooth, or it may radiate outward toward the jaw, ear, or even other teeth.
A day or two of tooth pain might not always signal a root canal. But pain that lingers for several days, keeps returning, or gets progressively worse is a sign your body is telling you something more serious is happening.
Why this can be a sign of root canal trouble
When the pulp inside a tooth becomes inflamed or infected, it puts pressure on the surrounding nerves. That irritation is what creates the persistent pain signal. Unlike sensitivity that fades quickly, this type of pain often doesn’t respond well to over-the-counter pain relievers for long. It keeps coming back because the underlying cause has not been addressed.
2. Lingering Sensitivity to Hot or Cold
Most people experience mild tooth sensitivity at some point. It’s often brief and resolves within a few seconds of removing the trigger. What separates ordinary sensitivity from a potential root canal warning sign is how long the discomfort lasts.
If you take a sip of hot tea or drink a glass of ice water and the sensitivity lingers for 30 seconds, a minute, or even longer after you’ve swallowed, that’s worth paying attention to. The same applies to:
- Hot beverages like coffee or soup
- Ice water or cold drinks
- Cold air hitting an exposed tooth
- Sweet foods that trigger a prolonged aching response
When sensitivity becomes a red flag
Prolonged sensitivity often indicates that the nerve inside the tooth is irritated or that the pulp itself is inflamed. Healthy teeth shouldn’t continue to ache once the temperature source is gone. The longer the lingering sensation persists and the more frequently it occurs, the more likely it is that professional evaluation is needed.
3. Swollen, Tender, or Pimple-Like Gums Near a Tooth
Your gums can sometimes give you an early warning signal before the tooth itself becomes intensely painful. Swelling, tenderness, or puffiness in the gum tissue directly around one tooth should not be dismissed as minor irritation.
Some patients also notice a small bump on the gum near the affected tooth. It may look like a pimple or blister and can sometimes feel tender to the touch. A few people notice the area bleeds more easily when brushing or feels unusually sensitive.
What gum changes may mean
When an infection spreads beyond the tip of a tooth’s root, it can create inflammation in the surrounding gum and bone tissue. That pimple-like bump is called a dental fistula or abscess sinus tract, and it forms when the body is trying to drain infection. It’s a clear sign that the problem has progressed and needs prompt professional attention. Waiting in this situation is not advisable.
4. Tooth Discoloration or Darkening
Take a look at all your teeth in a mirror. If one tooth appears noticeably darker than the ones next to it, particularly if it has taken on a gray, brown, or yellowish hue, that visual change can be a meaningful clue.
Tooth discoloration from the outside, such as surface staining from coffee or wine, tends to affect multiple teeth and can often be addressed with cleaning or whitening. Discoloration that originates from inside the tooth is a different situation altogether.
Why a tooth may change color
Internal discoloration usually means the blood supply to the tooth has been disrupted or the pulp tissue has started to break down. This can happen as a result of trauma to the tooth, even old trauma you may have forgotten about, or from an infection that has been silently developing over time. The darker shade is the tooth reflecting internal damage. It’s a sign worth investigating.
5. Pain When Biting, Chewing, or Touching the Tooth
You might not experience constant pain, but notice that a specific tooth hurts whenever you bite down into food or press on it with your tongue or finger. Some people first notice this while eating something as soft as bread or yogurt. Others feel it only when chewing on one side of their mouth, which they may have been unconsciously avoiding.
Why pressure can make it worse
Infection or inflammation at the root of a tooth affects the ligaments and tissue surrounding it. When pressure is applied from biting or chewing, it compresses those already-irritated tissues and creates pain. This symptom suggests the problem has extended beyond the inner pulp and is affecting the root and surrounding structures. Surface-level decay typically doesn’t create pain with gentle biting pressure, which is what makes this symptom particularly telling.
6. A Cracked, Chipped, Loose, or Injured Tooth
Visible damage to a tooth is not just a cosmetic concern. Cracks and chips create an opening for bacteria to travel into the inner layers of the tooth, including the pulp. This can trigger infection even when the damage looks minor from the outside.
Trauma is also a risk factor even when the outside of the tooth appears intact. A sports injury, a fall, or even an accidental bite on something hard can damage the nerve inside the tooth without leaving an obvious crack or chip. In some cases, pain or discoloration from that trauma doesn’t appear until weeks or months later.
How damage can lead to root canal treatment
A crack extending below the gum line, a chip that exposes the inner dentin, or blunt trauma that interrupts blood flow to the tooth can all lead to pulp death or infection over time. If you’ve recently injured a tooth or notice that an older injury site is now sensitive or changing color, it’s worth having it evaluated even if it doesn’t hurt yet.
How to Tell Whether It Might Be a Root Canal Issue or Something Else
Root canal symptoms can overlap with other dental and medical conditions, which is part of why self-diagnosis isn’t reliable. Here’s a quick comparison of how similar symptoms might appear across different issues:
Cavity pain tends to be triggered by sugar or temperature but doesn’t usually linger as long or feel as deep as pulp-level pain.
Gum disease or gum irritation can cause swelling and bleeding, but the discomfort is typically more general and spread across multiple teeth or a section of gum rather than isolated to one tooth.
Sinus pressure can mimic toothache, especially in the upper back teeth, because the roots sit close to the sinus cavity. Sinus-related pain usually appears alongside congestion, pressure behind the eyes, and other sinus symptoms.
Temporary tooth sensitivity from whitening products, recent cleanings, or minor enamel wear usually fades within a few days without worsening.
Teeth grinding (bruxism) can cause widespread jaw soreness and generalized tooth sensitivity, but it typically affects multiple teeth rather than one specific spot. Interestingly, Dr. Burgdorf’s practice also offers TMJ disorder management and sleep apnea therapy for patients dealing with grinding-related issues as part of a whole-health approach to care.
The overlap between these conditions is exactly why getting a professional opinion matters. The correct diagnosis changes the treatment path entirely.
When Should You Call a Dentist Right Away?
Some symptoms require more than a wait-and-see approach. If you’re experiencing any of the following, contact a dental office as soon as possible rather than waiting for your next routine appointment:
- Severe pain that is getting worse instead of better
- Swelling in the gums, cheek, or jaw
- A fever alongside tooth or jaw pain
- A persistent bad taste in your mouth or bad breath that doesn’t resolve with brushing
- Visible pus or drainage near a tooth
- Pain that is disrupting your sleep or making it difficult to eat
These symptoms can indicate a spreading dental infection, which does not resolve on its own. In cases like these, seeking emergency dental care promptly is the right move. An untreated dental abscess can spread to surrounding tissue and, in rare cases, become a serious medical emergency.
What Happens During a Root Canal Evaluation?
One reason people delay calling the dentist is anxiety about what the appointment will involve. Understanding the process ahead of time can make it easier to take that first step.
At your evaluation, your dentist will start by listening. You’ll be asked to describe your symptoms, when they started, what makes them better or worse, and whether you’ve had any recent trauma or dental work on that tooth. This symptom history is genuinely useful diagnostic information.
From there, the dentist will examine the tooth and surrounding gum tissue visually and with gentle probing. X-rays are typically taken to see what’s happening inside the tooth and at the root tip. In some cases, the dentist may test the tooth’s response to cold or apply gentle pressure to assess sensitivity.
After reviewing all of that information, you’ll receive a clear explanation of what’s happening, what your options are, and what treatment is recommended. Nothing will happen without your understanding and agreement.
What Happens If You Wait Too Long?
Dental infections do not improve on their own. Waiting on a tooth that may need root canal treatment tends to make the situation more complicated over time, not less.
As the infection progresses, pain typically intensifies. The infection can spread to the surrounding bone and gum tissue, making treatment more involved. A dental abscess may form, requiring additional procedures to drain. In advanced cases, the tooth may no longer be savable at all, which means extraction becomes the only option. That opens the door to a separate conversation about tooth replacement, including options like dental implants, which, while excellent long-term solutions, involve more time and expense than preserving the natural tooth would have.
Early treatment is almost always the simpler, less expensive, and more comfortable path.
Root Canal FAQs
Is a root canal painful?
Modern root canal treatment is performed under local anesthesia, which numbs the area so you don’t feel the procedure itself. Most patients report that the treatment is far more comfortable than they expected and that relief from the pre-treatment pain is significant.
Can root canal symptoms come and go?
Yes. Pain and sensitivity can fluctuate, which sometimes gives people the false impression that the problem is resolving. The underlying infection or inflammation doesn’t disappear on its own, even during quieter periods.
Can a tooth need a root canal without constant pain?
Absolutely. Some teeth with infected or dying pulp produce very little pain, especially if the nerve has already died. Discoloration, gum changes, or findings on an X-ray may be the only indicators.
How long can you wait before getting treatment?
There’s no safe universal timeline. Some teeth develop serious abscesses quickly while others progress more slowly. The safest approach is to have any concerning symptoms evaluated promptly rather than waiting to see if they improve.
Is it better to save the tooth than remove it?
In most cases, yes. Your natural tooth is the best option for long-term function, bite stability, and jawbone preservation. Root canal treatment allows you to keep that tooth functioning for many more years when done in a timely way.
How do dentists confirm you need a root canal?
Diagnosis typically combines your symptom history, a clinical exam, X-rays, and sometimes additional testing like thermal sensitivity tests or bite pressure assessment. All of that information together gives the dentist a clear picture of what’s happening inside the tooth.
Concerned About Root Canal Symptoms in St. Charles, MO?
If you’ve been experiencing any of the symptoms described above and you’re located near St. Charles, Dr. Kevin Burgdorf, DDS is accepting patients at his practice at 2050 Bluestone Dr, just off Hwy 94. We serve families throughout St. Charles, including residents from the Historic District, Harvester, Frenchtown, the Lindenwood University area, Heritage, and Earth City.
Whether you commute through the Earth City Business Park, live near Creve Coeur Lake Memorial Park, or have students at St. Charles West High School, accessible, high-quality dental care is close to home.
Dr. Burgdorf completed a general dentistry residency at University Hospital in Cincinnati, bringing hospital-level clinical training to his private practice. That means patients with complex or anxiety-inducing dental concerns receive a level of precision and calm that goes beyond what a typical clinic offers.
For patients without insurance, the practice offers an in-house Dental Benefits Plan with no deductibles, no waiting periods, and no annual maximums, so nothing stands between you and the care you need.If you’re experiencing symptoms that concern you, the right next step is a conversation. Call the office at 314-291-9000 to schedule an evaluation.


